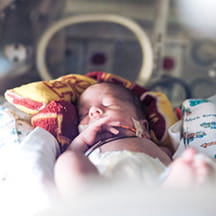
Caring for the most vulnerable populations in children often requires special tools, treatments or considerations. Research in children’s health faces unique challenges, including ethical concerns, fewer participants for studies, less funding, and longer approval time frames. Without the research and development from children’s hospitals, life-changing treatments wouldn’t be possible.
Here’s an array of recent significant scientific and technological breakthroughs in pediatric health made possible by children’s hospitals and health systems.
Leading the way in gene therapy
Gene therapy corrects underlying genetic issues, curing conditions not previously treatable and diseases that demand extraordinary efforts. Children’s hospitals have been at the forefront of much of the research, and they continue tailoring pediatric-specific therapies for chromosomal disorders.
Duchenne muscular dystrophy
Research at Nationwide Children’s Hospital has led to the development of Elevidys, the first gene therapy to treat Duchenne muscular dystrophy in 4- and 5-year-olds. This is the second gene therapy developed at Nationwide’s Abigail Wexner Research Institute’s Center for Gene Therapy to receive FDA approval.
Artemis-SCID
In late 2022, 10 children born with Artemis-SCID, a rare genetic disorder leaving newborns without functioning immune systems, were treated with a new gene therapy. This treatment, pioneered by UC San Francisco, home to UCSF Benioff Children’s Hospital, allows researchers to treat patients with their own stem cells by adding a healthy copy of the Artemis gene to their harvested stem cells.
Spinal muscular atrophy (SMA)
SMA is the top genetic cause of infant mortality. The only FDA-approved gene therapy, Zolgensma, was tested in clinical trials led by Boston Children’s Hospital. At least 3,000 children globally have been treated with the therapy.
Blood disorders
Researchers at Children’s Hospital of Philadelphia have developed a proof-of-concept model that delivers gene editing tools capable of modifying diseased blood cells within the body. Standard treatment requires children to have chemotherapy and stem cell transplants. The gene editing tool would eliminate the need for such treatments, and it could expand access and reduce the cost of gene therapies for blood disorders.
Childhood cancers
The latest advancement in treating childhood cancer is chimeric antigen receptor (CAR) T-cell therapy, which genetically modifies a patient’s T-cells to enhance their cancer-fighting abilities. Many children’s hospitals have been at the forefront of new CAR-T developments for pediatric cancers, including Johns Hopkins All Children’s Hospital’s Center for Adoptive Cellular Therapy.
Pioneering new treatments
From in-utero surgeries to one-of-a-kind devices, children’s hospitals have developed and implemented some of the most advanced and difficult methods to treat or cure children, giving them unprecedented opportunities in life and paving the path for further breakthroughs.
In-utero intervention for VOGM
A team of specialists from Boston Children’s and Brigham and Women’s Hospital developed an in-utero intervention for fetuses with an abnormal arrangement of blood vessels in their brains called a vein of Galen malformation (VOGM). About 60% of infants born with the condition develop severe problems such as heart failure or hydrocephalus, often immediately after birth. Despite advances in embolization techniques in newborns, the mortality rate for those babies is roughly 40%.
This first-of-its-kind ultrasound-guided embolization deploys tiny metal coils into the affected vein using a needle-guided microcatheter. Surgeons insert the needle through the mother’s abdomen into the fetus’ brain. With this intervention, children with VOGM are less likely to need heart failure medications or surgery to treat the malformation. The treatment may also offer a solution for newborns with VOGM who otherwise couldn’t be treated.
World’s smallest pacemaker
A multidisciplinary team within Norton Children’s Heart Institute partnered with a device company to produce and implant the world’s smallest pacemaker in a premature child. The infant was born with congenital structural heart defects and complete atrioventricular block (CCAVB), which has a high rate of prolonged illness or death.
Most children with the defect receive a pacemaker once they meet a minimum body size. However, this infant was too small, weighing less than three pounds. The team at Norton Children’s worked with the device manufacturer to determine compatibility and obtain emergency authorization from the FDA. Then, they successfully implanted it during a two-hour open-heart surgery. The device measures 1.16 by 0.65 by 0.38 inches and weighs 0.18 ounces.
First-ever artificial womb to aid preemies
Of the one in 10 U.S. births that are premature, about 30,000 per year are critically preterm—younger than 26 weeks. Only about 30% of infants born at 22 weeks survive, and just under 56% survive birth at 23 weeks. An artificial placenta, designed by pediatric researchers at Children’s Hospital of Philadelphia, could transform care for severely premature babies. By mimicking the prenatal fluid-filled environment, this technology gives newborns a few weeks to develop their lungs and other organs. The lead researchers tested their product on fetal lambs, in which lung development closely mirrors humans.
The eight preterm lambs tested in the prototype were physiologically equivalent to a 23- or 24-week-gestation human infant. This system mimics life in the uterus as closely as possible, building on knowledge from previous neonatal research. There is no external pump to drive circulation, because even gentle artificial pressure can fatally overload an underdeveloped heart, and there is no ventilator, because the immature lungs are not yet ready to breathe in atmospheric oxygen. Instead, the baby’s heart pumps blood via the umbilical cord into the system’s low-resistance external oxygenator that serves as a substitute for the mother’s placenta in the exchange of oxygen and carbon dioxide.
Potential cure for spina bifida
Three babies were born after receiving the world’s first spina bifida treatment that combines fetal surgery with stem cells. The one-of-a-kind treatment, over 10 years in the making, could improve outcomes for children with this congenital disorder. The achievement was made possible by the CuRe clinical trial at UC Davis Children’s Hospital.
Clinical-grade mesenchymal stem cells were manufactured from placental tissue at the UC Davis Health’s Institute for Regenerative Cures. A 40-person operating and cell preparation team placed the stem cell patch directly over the exposed spinal cord of the fetus during an in-utero surgery.
One-second cancer therapy
The Proton Therapy Center at Cincinnati Children’s treated the first participant in the world’s first clinical trial of FLASH proton therapy for cancers of the bones and chest. FLASH is an investigational mode of radiation therapy administered in less than one second. Research suggests that FLASH may result in fewer side effects than standard forms of radiation delivery, and the clinical trial is testing the feasibility of FLASH to treat people with cancer.
The FLASH research may have far-reaching implications for how cancer is treated. The proton therapy center aims to establish a foundation for future potential trials in brain tumors, sarcomas, lymphomas, lung cancer and other malignancies to transform cancer care.
Expanding the horizon
Children’s hospitals are always leading, conducting and publishing research to advance children’s health. For example, Rady Children’s Hospital is currently involved in more than 890 research studies by some 230 investigators, including 200 active clinical trials. While the discoveries and developments from children’s hospitals are innumerable, here are five examples of new insights that affect the lives of children and may lead to new ways to treat or cure patients.
ALS
Researchers at Boston Children’s Hospital have identified proteins involved in the innate immune system that could be at the root of neurodegenerative conditions such as amyotrophic lateral sclerosis (ALS), opening the door to new potential pathologies to target.
Seizures
Research from Cook Children’s Health Care System could help precisely identify the parts of the brain that cause seizures in children with epilepsy, resulting in safer and more effective treatments.
MRSA
Methicillin-resistant Staphylococcus aureus (MRSA) is associated with high morbidity and mortality. Children’s Hospital New Orleans developed an inexpensive nasal decolonization regimen that decreased MRSA rates by 50%.
Peanut allergy
Children’s Hospital Colorado developed a skin patch that was shown to be effective in desensitizing children to peanuts and increasing the peanut dose that triggered allergic symptoms.
Genomics
Researchers at Rady Children’s Institute for Genomic Medicine estimate that screening every baby born in the U.S. for genetic disorders would save 15,000 lives annually. Rady Children’s has sequenced the DNA of more than 7,500 people, and researchers at Stanford Medicine sequenced and diagnosed a genetic disease in less than eight hours, a world record.
At the forefront of vaccines
Vaccines protect children and communities, and most vaccines require years of research and development to ensure a safe and effective product. Children’s hospitals often lead efforts to research, develop, test and distribute vaccines around the world.
VTEU
Cincinnati Children’s is one of only 10 Vaccine Treatment and Evaluation Units (VTEUs) in the United States. VTEUs have been at the forefront of investigating vaccines to prevent or control epidemics, such as swine flu, Ebola and COVID-19. Cincinnati Children’s served as a key site for the testing of multiple COVID-19 vaccines.
COVID-19
Texas Children’s Hospital Center for Vaccine Development and Baylor College of Medicine created and engineered a recombinant, protein-based COVID-19 vaccine. The low-cost, patent-free vaccine can be licensed by any vaccine producer, increasing access for low- and middle-income nations.
Rotavirus
RotaTeq, recommended for universal use in infants by the CDC, prevents rotavirus gastroenteritis in infants. The vaccine was co-invented by Paul A. Offit, M.D., director of the Vaccine Education Center at Children’s Hospital of Philadelphia.