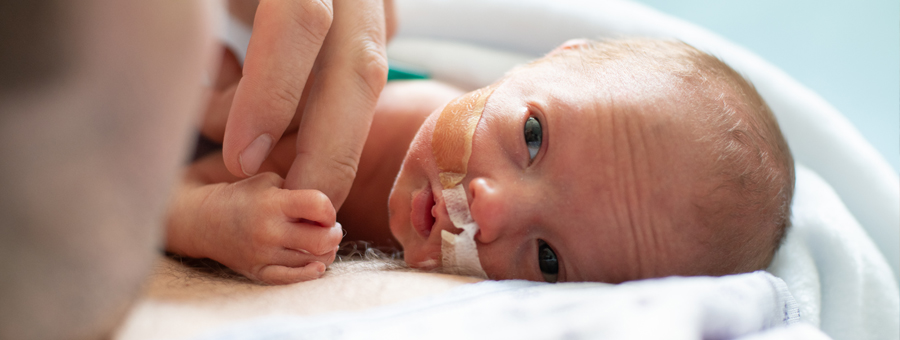
Rounding, improved hygiene and reducing the use of central lines helped Children's Mercy Kansas City go nearly a year without a central line-associated bloodstream infection (CLABSI) in its neonatal intensive care unit.
CLABSIs cause significant harm for patients of any age but pose a particular danger to NICU babies. Infections among this vulnerable population impact health outcomes and lengths of stay.
In early 2022, leaders at Children’s Mercy noted an increase in the frequency of CLABSIs in its NICU. Infection rates peaked at 3.88 per 1,000 line days in March.
“Our internal NICU goal is always zero CLABSIs,” says Annie Craig, MSN, RN, RNC-NIC, the hospital’s senior director of neonatal and perinatal services. “When we started to notice these upticks, we decided to address them as an interdisciplinary leadership team.”
Multi-tiered approach to reduce CLABSIs
To get to the heart of the issue, Craig and her team created a task force of medical directors, nursing directors, clinical nurse specialists and the quality improvement department.
The group found 75% of NICU CLABSIs occurred on double lumen central lines—those with two internal channels, or lumens. As a result, the task force asked patient care teams to use double lumen central lines only when medically necessary.
“A double lumen is nice, but it's not a need-to-have in most neonatal patients,” Craig says.
The Children’s Mercy’s CLABSI task force also worked to:
Reduce overall central line days. The task force recommended only using any type of central line when necessary and removing the line as soon as it was safe to do so.
Require parent handwashing. The hospital installed handwashing stations at its NICU entrances and required parents to wash their hands before entering.
Start high-risk rounds. A clinical nurse specialist, attending physician and bedside nurse began rounding several times each week on the NICU’s higher-risk central lines, including double lumen lines, those in precarious locations on the patient or those requiring frequent entries. As part of the rounds, the team met with NICU nurses to discuss safety interventions.
Communicate in group chat. The clinical nurse specialist team populated the NICU nursing team’s chat group with information regarding each central-line patient in the unit. Craig says this practice helped make nurses aware of patients with central lines as they started a shift and prompted discussions that led to fewer overall central line days.
Celebrate successes. Children’s Mercy staff members announce the number of CLABSI-free days in every team huddle, and it’s published in the clinical team’s weekly safety email to employees.
Processes drive CLABSI-free streak
The interventions led to an impressive streak of 332 days without a CLABSI in the hospital’s NICU—nearly double its previous longest run. Reducing the overall number of central line days was instrumental to that success, Craig says. Between the heightened priority placed on central line usage and daily discussions around patient cases, the hospital was able to decrease total central line days in the NICU by 40%.
Craig credits the entire organization for the accomplishment, saying support from hospital leadership and employee buy-in helped drive process changes. A bonus: the strategies decreased CLABSIs in the NICU can be applied across the organization and beyond, Craig says.
“These are principles that really could apply to PICUs, CICUs, med surg floors—anywhere that uses a central line,” Craig says. “These interventions didn't require new technology and besides the hand-washing sink, they were free. They were simply time-invested, collaborative and communication-invested interventions. They can be applied to different settings outside of the NICU—that’s what excites me most.”