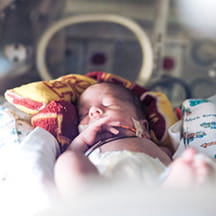
Sean Antosh and his team at Dayton Children's Hospital in Ohio had already begun looking into ways to improve the patient experience for children with sensory processing disorders, autism and anxiety when he experienced the “aha” moment: a patient’s family asked him to turn off the fluorescent lights above the bed in their child’s pre-operation room.
“Some neurodiverse people can actually see the flickering in those lights; we can't perceive it, but they can,” says Antosh, M.D., pediatric anesthesiologist at Dayton Children's. “Basically, the child was sitting under a torture chamber the whole time. It was one of those moments where I was thinking, ‘Wow, there's so much more we need to know about this.’”
Parental input integral to program
The project began shortly after Antosh arrived at Dayton Children’s in 2016. One of the pre-operative nurses there had a teenage son with severe autism and would tell Antosh about her experiences and the challenges a hospital environment can present for children with sensory processing disorders. There wasn’t much research available on this topic at the time, so Antosh and the child life team relied upon patient and family feedback to build a sensory program to meet the unique needs of this patient population.
“The parents’ voice is our number-one resource,” Antosh says. “They know their child best, so listening to them is the top priority we try to instill here.”
Heeding the advice of their patients’ parents, the sensory program at Dayton Children’s includes:
- Coping plans. Prior to a scheduled procedure, a child life specialist reaches out to families of patients who may require a sensory-friendly experience to understand their triggers and calming mechanisms. They use this information to develop a coping plan that resides in the patient’s EMR profile for the entire care team to reference.
- Sensory-friendly pre-operation rooms. Specifically designed to be quiet with low, soothing lighting and calming objects tailored to each patient’s needs, these rooms include color-changing floor tiles, fidget objects, weighted blankets and personal headphones.
- Calming surgical environment. Medical equipment and surgical instruments are covered or hidden as much as possible in the operating and recovery rooms to ease patient anxiety. Additionally, these areas have calming images on the ceilings and are kept as quiet as possible.
The sensory program has expanded over the years and now includes specialized rooms in other areas of the hospital, including the laboratory and imaging departments. Additionally, it’s now available to any Dayton Children’s patient who may benefit from the sensory-friendly environment—regardless of their neurological development or functioning.
Culture shift drives success
The sensory program has garnered excellent feedback from parents and has led to patients being referred to Dayton Children’s, according to Antosh. He and his team are in the process of publishing research to quantify its impacts on patient outcomes, but he’s already seen a dramatic improvement in one metric: the use of pre-surgery calming medications for patients has dropped from 90% of procedures to about 20% since the program’s inception. As a result, patients emerge from surgery less groggy and calmer, aiding in their recovery.
The customized rooms and calming gadgets are the most visible elements of the program, but Antosh says its heart and soul lies with the team members who implement it.
“The rooms are great, but it's actually the culture change we've had here that is the most important part of the program,” Antosh says. “You must change the way you provide care. You can build these rooms, but if the staff doesn't understand how to use them—or doesn’t listen to the parents—they're not going to be as functional.”