Simulation-based training has been around for centuries, but in the past 20 years it has grown exponentially. The role it plays in education is essential to enhancing both clinical skills and patient care while moving the needle on persistent quality and safety issues.
Studies show that education through simulations, both virtual and in-person, enables guided teaching experiences in a safe environment, accessible learning opportunities and a standardized assessment of skills. A hands-on approach to education also produces longer-lasting knowledge and skills.
“When you give a lecture, people learn things, but it’s usually not as much and not as sustained,” says Samreen Vora, M.D., medical director of the Children’s Minnesota Simulation Center. “Simulation helps people build muscle memory and better behaviors through practice.”
Children’s hospitals are innovating their simulation programs to fit the specific needs of their patients, communities and employees. Whether it’s technological advances, such as the use of augmented reality and 3D printers, or new courses to match a commitment to diversity, equity and inclusion, educators are providing resources to make patient care safer.
Augmented reality: Making life-saving simulations accessible
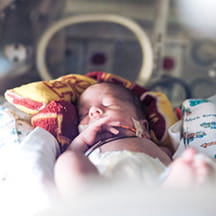
In rural Maine, difficult births led to some long-term health disparities when compared to their urban counterparts, according to one study. In hospitals with fewer than 500 delivieries per year, as opposed to those with more than 1,000, babies born needing resuscitation had a higher incidence of resulting brain injury. “It doesn’t seem fair that babies born in rural Maine are more likely to have a poor neurological outcome if they need resuscitation,” says Michael Ferguson, M.D., pediatric intensivist at Barbara Bush Children’s Hospital at Maine Medical Center in Portland.
When babies are born, about 1% to 2% need intensive resuscitation. This is a more frequent occurrence for hospitals that deliver 1,000 babies or more in a year. However, many hospitals deliver far fewer babies and only need to use intensive resuscitation every three to four years. “We know that if you don’t practice something every three months, you lose skills very quickly,” says Ferguson. “So, the simple answer is to have providers practice these skills regularly with simulation.”
However, simulation labs can cost a quarter of a million dollars or more to operate. “Where does a rural hospital come up with those funds?” says Ferguson. “They just don’t. They don’t do simulations because they can’t.”
After brainstorming how to bridge this gap in access and care, Ferguson and his team landed on augmented reality (AR) simulation as an affordable, portable solution. The simulation acts out a real-time neonatal distress scenario using an AR headset, a basic mannequin and a tablet—a “simulation lab in a suitcase,” as Ferguson calls it. An AR simulation blends the real-world environment—by practicing techniques on the mannequin—with visual and digital elements in the virtual reality headset, such as a baby’s coloration or other presenting factors.
With this gear, providers from anywhere can practice intensive resuscitation regularly. The simulation center at Barbara Bush Children’s Hospital serves as the central hub, and participants can access their AR simulations remotely.
Beyond accessibility, AR makes some aspects of the simulation more realistic than mannequins, like a baby’s coloring, breathing habits and movements. It also removes logistical barriers such as space requirements and reset and cleanup after a simulation, allowing more people to practice more frequently.
Currently, the simulation includes practice on a premature and full-term baby, but Ferguson hopes to expand the program to include resuscitation on a full-term baby, small child and teenager.
The project started before the pandemic with philanthropic donations and grants from the Innovation Center at Maine Health. As the program developed, it was tested by providers across Maine Health. Programmers and learners alike had to learn how to adapt to the headsets and lessons.
With topics like intubation, they had to learn to blend and manipulate the holographic part—what they’re seeing in the headset—with the physical component, which is what they’re practicing on the mannequin. “There’s a learning curve at first for people,” says Ferguson. “What you’re seeing in the glasses isn’t really there, so we have to sort of tease it out a little.”
The first set of simulation cases started to roll out to hospitals in late winter of 2022. “We know this does not replace high-fidelity simulation,” says Ferguson. “But we’re trying to give these hospitals an almost equal experience and education.”
3D printing: Customizing simulations refines care
Arkansas Children’s is home to the Simulation Education Center, with the mission of increasing safety, improving skills and promoting development.
Because children’s hospitals perform services on smaller patients and need specialized materials, they require far more customized simulations to improve applicability to real patients. One essential component to achieving that realism is the health system’s eight 3D printers. Ranging from basic to complex, the printers provide pediatric materials for both clinical and educational needs across the hospital.
“A decade or more ago, it was clear that there were unmet needs in the pediatric simulation space,” says Eric Braden, simulation specialist at Arkansas Children’s. “Most research and development comes from the military or adult hospitals, and the market segment for pediatrics is just smaller, so materials are often lacking in quality or availability.”
3D printing provides custom, high-fidelity models of anatomical parts, down to the tiniest of sizes. Using various materials, including synthetic resins and complex substances, they can print body parts such as limbs, hearts and spines that mimic the texture, density and size of the anatomical part. And they often only take a few hours to produce, depending on the model.
“We can print a mold to make realistic and anatomically accurate reusable models for a fairly low cost,” says Braden. The replicas can be used to enhance all kinds of simulations. Clinicians and educators across departments come to Braden with requests, and he produces lifelike aids to meet their simulation needs. “Faculty are often involved in the development of the model as well, so they have personalized input on what they need and what they want to do,” says Braden.
"We can print a mold to make realistic and anatomically accurate reusable models for a fairly low cost."
For example, the education team at Arkansas Children’s discovered that the options for pediatric central line training devices were lacking, and they were able to create custom devices that allow for repeated, simulated practice. In another case, they printed soft tissue molds using silicone or gels to add on to a mannequin to practice cannulation techniques.
3D printing is transformative for surgeons with patients who have congenital heart defects. Surgeons work with Braden to print and develop a model of a specific patient’s heart, which varies anatomically from person to person. Surgeons note that simply the tactile nature of the organ helps considerably, but the 3D models are so detailed—showing the exact structure of the heart with color-coded valves, arteries, and ventricles—that surgeons can develop a precise plan for the surgery, fabricate patches and other necessary materials ahead of time, and simulate the entire surgery on the model.
Recently, a surgeon at Arkansas Children’s was able to determine a more specific surgical plan with the patient-specific model of a congenital heart defect. “They were able to improve the patient’s quality of life long-term with a more complex repair, whereas before it was more of a simple repair,” says Braden.
Another benefit of a 3D model is explaining surgical plans to patients and families. Having a 3D visual of the organ helps them more readily understand the procedure than a 2D image does. In the future, Braden and his team hope to expand the program to help educate parents. One example includes patients who receive tracheotomies. Currently, their parents may go through training on a doll or something more generic. A 3D printed model would allow for more accurate training in case they have to perform the procedure in an emergency setting. “We’re meeting an absolutely unmet need,” says Braden.
Professional actors: Mitigating bias at the bedside
Over the past two decades, mounting evidence has revealed a pattern of implicit bias and inequities in health care. Though the detrimental effects of bias have been demonstrated, its unconscious nature makes it difficult to address and overcome. “No one shows up to the bedside planning to treat people differently, but the data shows that does happen,” says Vora.
While children’s hospitals have committed to improving this issue, it was brought to the forefront of Children’s Minnesota’s mission in 2020 when George Floyd was murdered in the neighborhood of the hospital’s Minneapolis campus. As an organization, Children’s Minnesota pledged to advance equity across the hospital system through a variety of strategies.
One facet of this work includes simulation-based training to help health care professionals reduce bias in patient experiences. “We started looking to see if there were things already being done, maybe not even in health care, that we know influence and change behaviors,” says Vora. “And that’s what simulation is perfect for.”
Vora and Brittany Dahlen, clinical education specialist at Children’s Minnesota in Minneapolis, created the Role of Bias at the Bedside simulation course. The four-hour program runs two to three times a week with groups of six to eight employees, clinicians and providers. It’s a live, interactive play-pause course that uses actors and scenarios to learn about and mitigate personal biases.
“We’ve built these cases and the course with actors from our community and partnered with a lot of stakeholders across Children’s Minnesota,” says Dahlen. “We wanted this work to be in line with the framework that the organization put forth, but also what our employees see at the bedside.”
"No one shows up to the bedside planning to treat people differently, but the data shows that does happen."
To build the course, Vora and Dahlen pulled information from community partners and employee resource groups, such as the Nurses of Color group at Children’s Minnesota. Employees voiced a need for more resources on subjects such as de-escalation, bias mitigation and validation tactics.
Using the hospital’s data stratified by race allowed the education team to home in on specific areas to start building their course. One scenario includes a Black mother in the neonatal unit who feels left out of the care decision making process. Participants then work with the mother, played by an actor, to validate and understand her feelings and agree on a path forward.
“When they interact, we’re having them focus on evidence-based, implicit bias mitigation strategies,” says Dahlen. “The facilitators are helping them identify what the concerns are that this caregiver is wanting to share.”
Another important consideration was the makeup of each group, including the participants, actors and facilitators. For example, they had to balance the power dynamics of each group to support everyone’s emotional safety, particularly people of color. The demographics of the group, based on managerial level, gender or race, can influence the way an individual may navigate the course. “This work requires a lot of emotional labor,” says Vora. “So, it’s important to debrief often throughout and at the end of the sessions. The facilitators also go through over 16 hours of training.”
The play-pause simulation format means that participants can pause the scenario to discuss the situation and how to move forward with input from the group. “We also let the actors regroup their thoughts and they come back to provide feedback to our learners,” says Vora.
Vora and Dahlen have committed to finding actors from the Twin Cities community. They’ll visit local theatre productions or work with acting troops to find individuals willing to offer their expertise and commitment to reducing bias. “They’re from our community and their feedback is so critical to the work,” says Vora. “Despite initial recruitment challenges, when we started looking in the right places, that is where we go, which has been incredible.”
In launching the course, Vora and Dahlen worked with leaders across the organization and the nurses’ collective bargaining unit to start with specific areas or teams. “We wanted this to be a shared language that people can use across the organization and within their teams,” says Dahlen.
The results have been overwhelmingly positive. Since 2020, more than 300 staff have completed the bias mitigation training. Participants take a situational judgment test where they respond to different scenarios, and their scores show significant improvement after taking the course. Through pre- and post-surveys, 95% of participants said they found it beneficial, and learners pointed out that they consistently use the strategies they learned during the course even three to six months later.