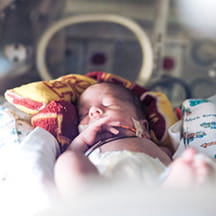
In many ways, J.J. Andreasen is a typical 13-year-old boy. He enjoys soccer, playing with friends and sharing his silly sense of humor. But when the otherwise-healthy boy suddenly developed acute liver failure in October 2022, he became a medical pioneer—the first U.S. pediatric patient ever to receive a liver transplant using normothermic machine perfusion (NMP).
“When he came in, he was so sick—I was really worried,” says Christine Hwang, M.D., pediatric transplant surgeon at Children’s Health in Dallas, Texas. “I was wondering if he was too sick to transplant and if he would make it through the surgery.”
J.J.’s best—and perhaps only—chance at survival was a transplant surgery with an NMP-preserved liver. NMP is an FDA-approved device that preserves the organ with warm oxygenated blood at 37 degrees Celsius, as opposed to the traditional hypothermic preservation method. The technology is relatively new but has shown promise in preserving organs for longer periods of time with reduced chances of damage. With NMP, doctors can monitor liver function prior to transplantation so it can be transplanted with fewer adverse effects for the patient during the operation, which was crucially important in J.J.’s case.
“He was intubated, he was on MARS (Molecular Adsorbent Recirculating System), which is essentially artificial liver support, and he had a lot of swelling in his brain, which concerned us very much,” Hwang says. “We didn't want anything to happen during the surgery that might cause any big shifts in his blood pressure that could potentially affect the pressure in his brain.”
The success of NMP
Today, J.J. is thriving. His transplantation surgery went smoothly, and his recovery has been remarkable—he was discharged from the hospital in less than a week and has now returned to school. Hwang credits NMP technology with the success of J.J.’s liver transplant surgery and the speed of his recovery.
Meanwhile, research into the benefits of NMP is ongoing. One recent study shows NMP enabled surgeons to assess and successfully transplant 15 of 21 adult livers that otherwise would have been discarded as unsuitable. Those results, along with the longer storage timeframes provided through NMP storage, could help reduce lengthy patient waitlists for organ donors. Hwang is hopeful these positive developments can counter the higher costs associated with NMP transplants, and J.J.’s amazing outcome can help contribute to wider application for children needing liver transplants.
“We did a study of our adult patients who were transplanted with NMP, and they averaged a shorter length of stay. Even though there's a cost concern I would argue with the shorter hospital stays you can recoup those costs,” Hwang says. “This is great technology—it has a lot of benefits, and I think it will increase the number of organs available to our pediatric patients.”