Listening to an interview chronicling the raid of Osama bin Laden's compound in 2011 by the U.S. Navy's Sea, Air, and Land (SEAL) Team Six got Jason Foland thinking about pediatric emergency care.
Foland was fascinated by the six months of rigorous training the SEALs endured for this singular event—planning exhaustively to respond to any unexpected turn the mission could possibly take.
"With that in mind, I wanted to practice and simulate all the high-risk scenarios we encounter," says Foland, M.D., pediatrician-in-chief, The Studer Family Children's Hospital at Ascension Sacred Heart in Pensacola, Florida.
"As a pediatric ICU physician by training, I recognize how scary it can be for non-emergency providers to take care of children. So, while Seal Team Six was the inspiration behind this program, I've always had a passion for this kind of thing."
Realism changes the game
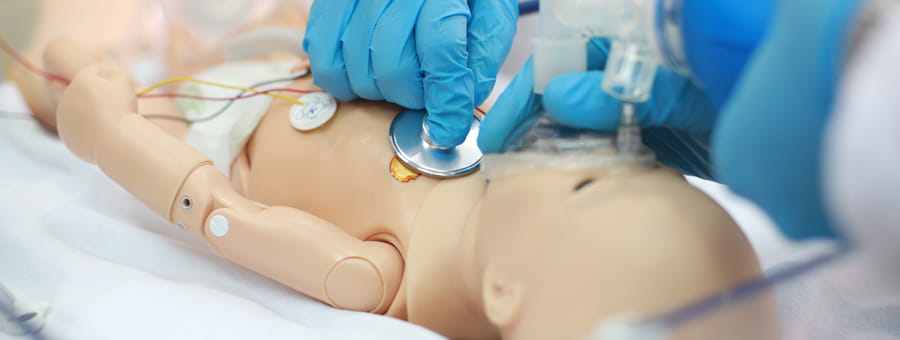
To build his vision, Foland secured funding for three training mannequins to simulate a newborn, a 6-month-old and a 9-year-old. Foland says they're incredibly lifelike; among the physiological conditions, they can simulate are crying, eyes that open and close, pupils that dilate, variations in heart rate and respiratory function and even seizures.
Foland and his trainers control the mannequins wirelessly to simulate these scenarios; he says the realism allows practitioners to immerse themselves in the simulations.
"You have to treat these dolls like real patients," Foland says. "In the past—with lower-technology mannequins —, I might say 'the child is wheezing,' but now I can make the mannequin wheeze and the caregiver in the simulation actually has to listen to the mannequin with their stethoscope and interpret the sounds coming out of it."
Curriculum allows for customized training sessions
Foland, along with his team of seven mannequin training specialists, created a curriculum with the aim of keeping providers' skills sharp while getting them more comfortable with emergency situations they may not see on a regular basis.
The team conducts several training sessions per week—to date, more than 400—with groups of providers throughout the children's hospital, in other health care facilities in the Ascension Sacred Heart network and with first-responder agencies in the region.
In addition to addressing basic life support skills, the training covers advanced scenarios with a focus on early recognition of children in distressed states to avoid a full-code situation.
Each training session is tailored to the skill level of the audience and its needs. Prior to a simulation session, Foland's team pulls coding data from that unit to determine its most common diagnoses and emergency situations to customize the mannequin simulations. And to ensure maximum effectiveness, the sessions are held in that unit's clinical spaces rather than a conference room or designated training room.
"By simulating in their environment, we find things in their processes of care that may need to be improved," Foland says. "It helps identify things they need to do to provide better quality and safer care."
Foland says those improvements have included helping clinical teams redesign workspaces and relocate supplies to maximize effectiveness in a crisis. The simulation team also customizes their sessions around recent events and seasonality—for example, with the warmer weather, Foland and his team have focused on drowning scenarios.
Feedback, results from program are positive
Foland says staff feedback on the program has been overwhelmingly positive. It takes about eight to 12 weeks for his team to complete the rotation through all eligible staff members—and he finds providers are eager to revisit the training once they've gotten a taste for it. "It's like a glass of water in the Sahara," Foland says. "People are really thirsty for it."
He's also seeing positive effects on patient care. Everyone appears to be more comfortable, and less-experienced practitioners are taking more active roles in emergency situations, according to Foland. He adds communication in those scenarios has gotten much better, as everyone on the team can anticipate the needs of the others.
"It's so gratifying because you want to share this knowledge when it's not an emergency—it really changes the stress level of the education, and ultimately everyone's prepared when they actually see an emergency," Foland says.
"The reason we're doing this is because we love these children, and we want them to have the best care possible—the people doing this are doing so out of dedication to take care of kids."