Over the last five years, teams at Spectrum Health Helen DeVos Children’s Hospital in Grand Rapids, Michigan, had completed at least four different improvement projects focused on increasing adherence to the independent double check (IDC) process.
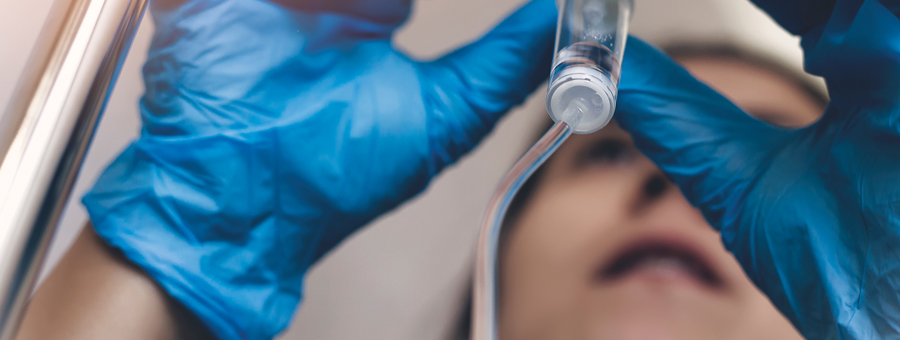
An IDC is when two registered nurses independently check a medication to ensure it is correct prior to administering it to the patient. Like other institutions, the hospital did not require this process for all medications but did require it for a select group of medications considered higher risk if given in incorrect doses, routes or times.
For years, the hospital examined and analyzed the process and related policies for administering these medications, but with no appreciable change in medication error rates. The latest efforts included reducing the number of medications that required an IDC, which pleased the nursing staff, but still did not fix the issue.
Then, in the summer of 2019, a medication administration error in the PICU triggered yet another root cause analysis of the IDC process.
The frustration of repeated analyses and efforts led the team to take a different approach to investigating its practices. They leveraged the expertise of a resident human factors practitioner—an expert in evaluating the interactions of people, tasks, the environment and technology—to lead the analysis.
The root cause analysis team, in partnership with the human factors practitioner, was tasked with understanding the PICU’s IDC practice and what might be done to strengthen it. Little did they know their investigation would lead them to ask broader and different questions about IDC than they could have imagined.
They went from wondering how to do an IDC better to wondering why they were a good idea in the first place. This realization came from examining unsatisfactory data and misguided theories on how humans interact with their work environment and each other.
Find the barriers
The human factors practitioner facilitated a team of nurses, pharmacists, corporate medication safety specialists and nurse leadership. They captured the current state of the PICU work system to complete a human-centered work systems analysis.
The findings were visualized using the Systems Engineering Initiative for Patient Safety (SEIPS) model, which gave the team the ability to identify the barriers or enablers to the IDC process.
The plan was straightforward: Find what barriers existed in the work environment and create a plan to address them. After the analysis was complete, however, the team identified so many barriers to the process that they wanted to conduct a deep dive into the nursing literature.
They wanted to understand whom they could learn from—who was having success and could advise on the best way to address the barriers impeding completion of the IDC process. The team was surprised to find, at best, there was inconsistent outcomes data to support the use of the IDC, and there was even a smattering of articles suggesting the practice may not be worth the effort and needed more review.
The Institute for Safe Medication Practice (ISMP) published a white paper recognizing the challenges to effectively performing an IDC but maintained it is a worthwhile practice by citing articles in support of it.
The challenge for the team, however, was the cited research articles lacked high-quality supporting evidence, with none of the studies conducted on a nursing unit. The paper hedged in its conclusions by suggesting organizations should consider whether they should adopt the practice or consider something else.
This paper, combined with the lackluster outcomes data in nursing literature, led to another deep dive, but this time into the human factors and resilience engineering literature. This work changed the course of the project.
Human factors science
After exploring the human factors and resilience engineering literature, the team members were able to understand why it seemed so difficult to adhere to, and gain benefit from, the IDC process.
First was the finding that double-checking as a practice seems to have its roots in resilience engineering theories on positive redundancy. This is the idea that if you have a safety-critical step, it is prudent to build in redundancy as a fail-safe. This is logical and easy to understand, but the catch is that this theory is based on pure technical systems (just technology), and not sociotechnical systems (people plus technology).
There is nothing in the literature or theory to suggest such a practice should be applied to people. Yet we do so as common practice in many settings with the assumption that all forms of redundancy are equal—they are not.
The second finding took the team a step further to understanding the emergent effects of redundancy in sociotechnical systems: social loafing. Social loafing is a well-documented social phenomenon observed when two or more people are working on the same task.
It describes how, quite unconsciously, people will not try as hard if someone else is checking their work. Viewed from this perspective, the IDC could be a possible detractor of safety rather than a booster of it, and any “good catch” a second person makes would have been less needed if they were not there in the first place. That is, the first person is more apt to make an error if the second person is there.
The final finding involved the efficiency, thoroughness, trade-off (ETTO) concept. This principle further details the social loafing phenomenon by explaining that humans seem to only work in one of two modes, efficient or thorough.
The mode they choose depends on (generally unconscious) rationalizations of risk: “I can afford to be fast (efficient) at the expense of being thorough because the other people in this process will be thorough,” or, “I cannot afford to be fast and not thorough, because it is just me here.”
ETTO is on display when people are working in resource-constrained environments doing teamwork, which is nearly all real-world work situations, especially in nursing units. This consideration helped the team see how a nurse’s brain might be working when administering a medication, especially one that was prepared in the pharmacy, barcode scanned, checked by someone else, or all of the above.
Forced dual signoff
The team began gelling around the idea the IDC was not the safety measure they thought. They began to look at their policies in a new way, especially the codification of policy in the EMR. The EMR had a function called a “forced dual signoff.”
Once an IDC medication is scanned, the computer locks on that screen until a second nurse signs off that they double-checked the medication. If a second nurse does not sign off, the computer remains locked, rendering it unusable until signoff occurs. The team did a quick-time study to determine the amount of time it took nursing staff to perform an IDC (and thus prevent having the computer locked out).
They found that while performing one IDC, it took nurses between two and 32 minutes, with an average of 7.5 minutes, to find a second nurse. This means not only was the medication administration delayed for that amount of time, but the nurse’s computer was locked during this time too.
Once a second nurse was found, the amount of time it took nurses to document an IDC medication was between 5.25 and 8.5 minutes due to the number of pages and tasks that must be clicked through.
Viewed with the ETTO in mind, this forced dual signoff only added to the time constraints of nursing staff and decreased the likelihood they would operate in thoroughness mode while administering a medication.
Returning to single-checks
After discussing the findings, the team decided to pilot the return of single-checking medications in the PICU. The pilot excluded the cardiac ICU population due to the location of these patients in the hospital, and excluded total parenteral nutrition, lipids and chemotherapy because these medications have different staffing and processes.
PICU staff attended an in-person explanation of the pilot and process change via pre- and post-shift meetings. The Single Checking and Administration of Medications Scale (SCAMS-II) survey was administered to nurses, which assessed their attitudes toward IDCs and single-checking.
Prior to receiving education about the data and human factors behaviors, 58% of nurses favored single-checking medications. After the in-person education, 91% of nurses favored single-checking medications.
Beyond how it’s always been done
Prior to implementation, the hospital had a 1.21% rate of errors involving medications on the mandatory IDC list. In the year after implementing single-checks, the rate of errors involving IDC medications dropped to 0.78%.
The amount of time nurses spent finding a second nurse dropped by 95%. Searching for a second nurse only occurs now when a nurse has questions. This amount of time equates to roughly five hours of nursing time saved per day based on a half-full census. The amount of time it takes to document an IDC medication was reduced by 44%.
One year after returning to single-checking medications, 92% of nurses in the PICU continue to favor this process over double-checking medications, and 92% of nurses said they feel encouraged to ask questions about medications during the single-checking process.
The project’s outcomes show support for alternatives to safely administering medications without using IDCs. It can be difficult to challenge the status quo. But don’t forget the importance of looking at data rather than relying on processes that exist simply because that’s the way they’ve always been done.