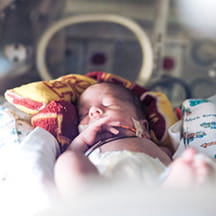
The year 2019 handed a series of challenges and changes to pediatric health care institutions. Measles made a comeback, requiring many providers to familiarize themselves with an illness that most people have only seen in textbooks. Vaping and a new area of care where a vaping-related illness may present as something else are making it difficult to implement the right care plan. And there's telemedicine. The care model, designed to conveniently care for patients where they are, has been around for years, but it's changing and growing all the time.
These areas are requiring children's hospitals to think about new ways of doing things—from delivering care to expanding programs. Here's a look at how three children's hospitals are doing just that.
Measles: Spread a message
For the better part of a generation, measles has been officially eliminated from the United States. Yet, 2019 saw the most measles cases since 1992. The vast majority of the more than 1,200 cases reported to the Centers for Disease Control and Prevention (CDC) last year, including outbreaks in 10 states, were among unvaccinated children:
-
339 cases were reported in kids ages 5 to 17 years old.
-
274 cases were reported in children 16 months to 4 years old.
-
277 cases were reported in children 0 to 15 months old.
This sudden influx presents a challenge to children's hospitals: how best to treat patients with a disease long considered to be dormant. "It's been quite a learning curve, because measles was essentially eradicated," says Rudolph Valentini, M.D., FAACP, chief medical officer of Children's Hospital of Michigan in Detroit. "I've been practicing pediatrics for about 30 years, and it was gone when I started—I never had it, nor did anybody I knew. It's just something that you don't encounter very often."
Treating measles requires caution
The U.S. achieved measles elimination status in 2000 and despite the 2019 outbreaks, maintains that distinction. But the dramatic jump in measles cases last year highlighted our vulnerability: international travelers bringing the disease back to large pockets of unvaccinated individuals.
For Valentini and his team at Children's Hospital of Michigan, dealing with this relatively unknown disease required an abundance of caution. "We learned the most from our index case to have a high level of suspicion for anybody with a fever, rash and a history of travel," he says. "You need to isolate that patient. You need to quarantine him or her right away so you can minimize the risk—it's OK to be overly cautious."
Given the highly infectious nature of measles, being "overly cautious" with that first patient means analyzing any instances where the disease could have spread. Valentini led a team that treated the hospital's first measles patient of 2019. "We had to track every step this kid took in the hospital, which elevator he got on, who else could've been in the hallway—including staff and the parents and families of other children," Valentini says.
"We looked at all the patients who were in close proximity to this patient and if they were immunocompromised—if they were on chemotherapy or on immunosuppressant medicines, we actually had to give them additional treatment."
Valentini adds that his team has even gone out to the parking lot to put masks on incoming patients who might be infected. Children's Hospital of Michigan has also considered assessing the vaccination status of hospital visitors to further reduce the risk.
Urging communities to heed their 'societal responsibility'
According to the CDC, the overwhelming majority of U.S. children are vaccinated against measles—more than 90% each year for the past two decades. But it cites misinformation about the safety of the vaccine in some communities as a reason for the outbreaks, particularly in New York, where more than 75% of all measles cases in 2019 occurred.
In Detroit, Valentini says he and his team have been making a concerted effort to spread the pro-vaccination message throughout the community and via the media. "My message is that getting vaccinated is the responsible thing to do—even if you don't do it for yourself, do it for your neighbor," Valentini says. "If you don't want to protect your own kid because you're afraid of something about the vaccination, think about everyone else—it's a societal responsibility."
Vaping: Focus on prevention
When the first two cases of a mysterious lung disease appeared at Children's Wisconsin in June 2019, Michael Meyer and his team had no idea they were on the verge of an epidemic. But as otherwise healthy teens continued to present with serious lung dysfunction, it was clear something was happening.
"Dr. Lynn D'Andrea was our pulmonologist on call at the time and was bringing the fifth kid back to the operating room for a bronchoscopy," says Meyer, M.D., medical director of the pediatric intensive care unit at Children's Wisconsin in Milwaukee. "She told me, ‘This isn't infectious—there's something else going on. I don't know what this is, but it really has me worried.'"
The bronchoscopies were exacerbating the symptoms, and the patients weren't responding to traditional treatments. But a common thread emerged: All had reported vaping or using e-cigarette products. "That is where it all came together," Meyer says.
Sudden spike in lung injuries poses challenges
Meanwhile, a similar scene was beginning to play out around the United States. The cases at Children's Wisconsin were still somewhat of an anomaly in early summer—only 67 cases of e-cigarette or vaping product use associated lung injury (EVALI) had been reported to the CDC through June 2019. But that number would soon skyrocket.
As of late December 2019, nearly 2,500 EVALI cases requiring hospitalization had been reported across the country, including 55 cases that resulted in death. About 15% of the EVALI cases involved children under 18 years old. For children's hospitals, the sudden onslaught of serious lung injuries due to vaping presents a variety of treatment challenges:
Uncovering e-cigarette use. Although vaping may be suspected, a teenager may be hesitant to disclose that information—especially in front of his or her parents. "Telling the truth can be scary for them. I don't think it's always intentional, but I think there's some embarrassment," Meyer says. "There's denial that it's a problem."
Black market products. Even if the patient is willing to divulge a vaping habit, he or she may not know what they've inhaled. There's a flood of bootleg products that can be used with e-cigarette devices, many containing harmful chemicals including THC, cannabinoid (CBD) oils and vitamin E acetate. "This behaves likes smoke inhalation. It's some type of chemical particulate matter, whatever it is, that causes this damage," Meyer says. "One of the biggest challenges from a health care provider standpoint is understanding that people are willingly doing this to themselves."
Lack of information. The rapid acceleration of vaping-related injuries forces health care professionals to treat with relatively little historical background. "We're still at the very early stages of understanding the science around this," says Michael Gutzeit, M.D., chief medical officer and chief safety officer at Children's Wisconsin. "The exponential use of it within just the past three to five years has created a vacuum in terms of knowledge."
Vaping a "national epidemic"
E-cigarettes typically contain substantially more nicotine than combustible cigarettes—one Juul pod contains as much nicotine as 20 cigarettes—so addiction is even more likely. "One of the struggles we're having is that some of these kids have continued to vape even after being hospitalized with a serious illness," Meyer says.
"I think a lot of them are addicted to the nicotine."
Meyer and Gutzeit agree prevention is the most important priority to combatting this concern. And they say children's hospitals can play a pivotal role in stemming the tide. "It's really where our focus is heading right now, because I think this is a disease that's 100% preventable," Gutzeit says. "If you don't vape, you don't get vaping-associated lung injury."
Meyer adds, "This is truly a national epidemic and a public health concern that rises to the level of any other serious illness that exists in the country."
Telemedicine: Determine the need
It's a health care challenge that probably dates back to the days of Hippocrates himself: how to coordinate the medical needs of all patients with a finite population of clinicians—often when the two parties are separated by great distances. Children's hospitals are increasingly turning to telemedicine to bridge the geographical gap.
Organic growth for telemedicine program
Aaron Martin, M.D., now the telemedicine medical director at Children's Hospital New Orleans, began using telemedicine in early 2017 as a tool to care for his remote urology clinic patients. Soon, other specialists at the hospital began requesting the technology. Today, Children's Hospital New Orleans' patients across about 20 specialties benefit from virtual care.
"I believe that's been the source of our success. It's really been the physicians who have driven this model," says Amanda Jackson, M.D., medical director of primary care at Children's Hospital New Orleans. "It's just been the physicians responding to their patients' needs."
Statistics point to telemedicine growth
Jackson says concern about reimbursement was a focal point as Children's Hospital New Orleans looked to build its telemedicine program. "When we started, we were specific about doing telemedicine within the state with our providers where we had payer contracts and our Medicaid was reimbursed," Jackson says. "We looked at this strategically to ensure there would be minimal financial impact to the patients, and we would be able to work with our payers to get reimbursement for the program."
Nationally, the recent expansion of telemedicine programs suggests the technology's usage is poised to explode:
- A national study of insurance claims shows telemedicine usage shot up 53% from 2016 to 2017 alone, according to a report published last year by Fair Health, a nonprofit that operates a vast database of commercial and Medicare claims.
- A 2017 Nemours Children's Health System survey of its patients' parents—compared to a similar survey conducted just three years earlier—showed the use of online doctors' visits had grown by 125%, and parents' awareness of telemedicine services had increased 88%.
- A Global Insights report projects the telemedicine market will expand from $38 billion in 2019 to more than $130 billion worldwide by 2025 with the U.S. accounting for half of that global market.
For the second consecutive year, the U.S. Centers for Medicare & Medicaid Services expanded reimbursements for remote care services in 2019, paving the way for further telemedicine growth.
Telemedicine serving multiple health care uses
For Children's Hospital New Orleans, expanding its telemedicine footprint has meant evolving the program from specialty clinics to an after-hours clinic, urgent care, primary pediatric care and a school-based program. "It's really just been determining what the need in the community was and responding, so we could deliver care where the patients were," Jackson says.
Delivering care directly to the patients has proven most effective at the school level—something school nurses often appreciate as much as parents. "We would like to be able to do as much as possible in the school setting so the kids can remain in school—to continue learning while we are ensuring that their medical needs are met," Jackson says. "The school nurses are so grateful to have the secondary support from a health care provider to back them up when there are questions or concerns about the kids who are in school."
Jackson adds that future expansion of telemedicine at Children's Hospital New Orleans will likely be focused on delivering chronic care management in the school-based setting. "Things like asthma management where, if the child's not having acute flare-ups, we can ensure that she's getting asthma education and her medications are correct," Jackson says. "Asthma management is a great application of this technology."
What the public wants
Beyond the logistical benefits, patients are increasingly clamoring for more virtual health care options. A 2017 Harris Poll survey found two-thirds of American consumers would like to see their primary care physician (PCP) via a virtual visit, with 20% saying they would switch from their current PCP if another PCP in their area offered telemedicine services.
The job market is reflecting this demand. Doximity's 2019 U.S. Physician Employment Report lists family medicine and pediatrics among the five most highly sought-after specialties in the growing telemedicine field.
According to Jackson, interest in telemedicine is perhaps heightened among pediatric patients because they have grown up on the technology. "This is how they interface with their world—it's FaceTime, it is Snapchat," Jackson says. "They are talking to each other through their technology, so this is actually their preferred method of communication."
Jackson says having technology act as a buffer can make a virtual care visit more comfortable for a pediatric patient. "These kids get the safety and security of being at home—it's not embarrassing to talk about their issues," Jackson says. "And they don't have to experience that frightening feeling of being in a hospital."