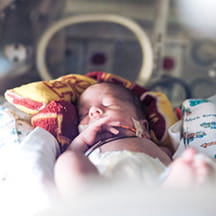
A newborn infant was unable to regulate his body temperature in the first few hours after birth. A nurse made an improvised heat pack of hot water from an instant hot water dispenser and tucked it under the newborn’s side to warm him.
The nurse was newly off orientation as a graduate, and her preceptor showed her how to make a heat pack for this purpose. She was unaware the temperature of the heat pack was too hot for the newborn’s fragile skin, and the baby suffered full thickness burns on his thigh and buttock area, requiring plastic surgery and skin grafts.
While this was not an event at Children’s Mercy Kansas City and it occurred 20 years ago, thermal injuries like this occur in hospitals every day and cause wounds, pressure ulcers, severe burns, blisters and scarring to pediatric patients.
Injuries occur when the appropriate products are not available to providers and they use an improvised device or when approved devices are used inappropriately. Injuries can also occur when products are misused or manipulated for pediatric use. Injuries from hot or cold thermal products can result in the need for wound care, antibiotic therapy or surgical intervention, in addition to the health issue providers were initially treating the child for.
The Child Health Patient Safety Organization® (PSO) identified concerns related to harm caused by thermal products and devices through data reported from PSO members. The group developed a risk assessment to help hospitals proactively identify organizational gaps. The thermal injury risk assessment—the first produced—covers nine areas hospitals can assess for potential issues that could lead to harm.
Within each area, specific elements to be assessed are listed, along with recommended risk mitigation strategies for each element. The assessment provides a mechanism for hospitals to prioritize areas of vulnerability. Questions help participants identify current gaps in their organization, and the assessment calculates a risk prioritization score. If participants identify a gap, they score the organization’s vulnerability based on three elements:
- The likelihood the cause of the gap would occur
- The effect on the patient
- How likely the organization would detect the gap when present
While this work is important for narrowing a hospital’s focus on the issue, obtaining buy-in from key stakeholders to complete and implement a risk assessment can be challenging. Hospital staff are often busy with direct patient care needs, and this can leave little time to implement proactive safety work. Here’s how Children’s Mercy navigated the challenges of implementing change and used a committee structure to conduct a thermal injury risk assessment and avoid pediatric harm in the organization.
Convey a powerful message
As Children’s Mercy began to investigate the use of thermal products and devices in the organization, areas of risk began to reveal themselves. The hospital used real safety stories like the one above, along with photos of thermal injuries, to get the attention and buy-in of stakeholders.
Sharing safety stories involving thermal injuries at morning huddles, hospital and unit committee meetings and as the monthly featured safety story, helped the hospital achieve buy-in to complete the thermal injury risk assessment and implement the resulting action plan. Once providers heard the stories and saw the pictures, they wanted to keep thermal injuries from occurring.
Put the assessment to work
Nurses are the primary users of thermal products and devices at Children’s Mercy. The chief nursing officer was instrumental in adding the thermal injuries risk assessment to the agenda at the Nurse Practice Council (NPC). NPC has authority over clinical practice standards for the Nursing Department and includes subject matter experts from areas where nurses practice.
To complete the portion of the risk assessment that identified any gaps, questions were presented to the group on slides one at a time. The NPC was asked to think about the question and identify any gaps, and participants were asked to answer the questions based on their individual perspective or experience.
If they identified a gap, the members were asked to elaborate while the information they provided was recorded in the risk assessment. Using this format, with over 50 members present, the hospital identified gaps in one hour. A subgroup from NPC was formed to complete the scoring portion of the assessment and prioritize gaps from highest to lowest risk.
Prioritize highest risk
Once the group identified the areas of highest risk based on the calculated scores, suggested risk mitigation strategies were put in place for the top five areas of greatest potential harm. Several disciplines became involved in this work, such as physicians, education, clinical safety and value analysis to implement the action items for each gap. The areas that posed the greatest potential for harm were:
- Identification of need and appropriateness for application of heat and cold
- Identification of thermal equipment and supplies approved for safe use
- Selection of device(s) for use
- Application of device(s)
Discourage use of improvised heat packs
One element of interest for the group was the use of improvised, makeshift heat packs. There are many reported ways clinical providers can make an improvised heat pack, which can cause burns and injuries. Some examples of makeshift items include:
- Using instant hot water from a dispenser or coffee pot, which can be as hot as 190 degrees.
- Filling a disposable diaper with instant hot water and placing it inside a plastic bag and sealing it with tape. The outside of the pack is then covered with a thin baby blanket or towel.
- Filling a pouch typically used to make an ice pack with a disposable diaper and then adding instant hot water and tap water.
- Wrapping towels soaked in hot water in absorbent pads and reheating them in the microwave when they cool off. In addition to causing burns, these can catch on fire or char the towels.
Methods used to make thermal products are passed down from provider to provider, so this type of unadvised practice becomes normalized. There are also unit norms staff members adhere to without recognizing the risk for injury involved when making thermal products for their patients. The problem with makeshift heat packs is there is no way to measure the temperature of the heat pack once it is assembled or reheated.
There are many reasons why providers use improvised heat packs. Many nurses believe the manufactured heat packs stocked on units do not get hot enough. There are products available on the market that reach a safe therapeutic temperature and then maintain that temperature for an appropriate amount of time.
Sometimes the manufactured heat or cold packs are not available on units because the amount of inventory needed is low, or they must be obtained from an area outside the unit. At times, these manufactured products or devices are not used because the staff members simply are not aware of the thermal products available in the organization.
Build an action plan
At Children’s Mercy, once the NPC subgroup identified gaps and recommended risk mitigation strategies, group members drafted an action plan. The group took the proposed plan, along with the thermal safety stories, to the Patient Safety Evaluation System (PSES) committee to gain executive support and plan approval.
PSES is comprised of several members of the executive team, clinical safety and risk management, and they have the leadership leverage to remove barriers, grant final approval and hold operational leaders accountable for completion of the action items. The action plan was approved with committee support.
Implementation of the action plan involved disciplines from many areas of the hospital. The group tapped into the Physician Safety Committee by enlisting the help of a member hospitalist. She was instrumental in using the thermal safety stories and thermal injury risk assessment results to achieve buy-in and collaboration with the hospitalist team. Physician feedback helped ensure standardization of order sets and device use for thermal therapies.
The value analysis team was key to ensuring there were adequate products in place on each unit. Value analysis updated the process for evaluation of products and devices as they were introduced into the organization. Education on the new products was part of the updated process and would ensure providers were knowledgeable on how to use thermal supplies and devices appropriately.
Although there is not one single action item that can be implemented to change a culture, several action items at Children’s Mercy brought awareness to thermal injury and began to shift the culture toward thermal safety. The NPC chairperson developed an education module for nurses and care assistants on thermal products that became a required part of annual education. The NPC subgroup evaluated current education resources for the proper use of thermal supplies and devices and updated them to incorporate the new risk mitigation strategies.
The work group collaborated with the biomedical engineering team to standardize all thermal products and equipment and ensure the nursing staff knew all the options available to them. Job aides with references made it easier for staff to do the right thing. These included a time and temperature relationship to severe burns and a list of approved thermal products available in the organization. The corresponding order number for products that are not already stocked on every unit were listed as well, making them easier to obtain.
Keep the momentum going
It took seven months once the hospital completed the thermal injury risk assessment to fully implement the action plan. Nearly two years have passed, and the hospital has not had a single thermal injury report. The work group continues to monitor for thermal injuries, and members are actively trying new ways to operationalize risk assessments.
Members of the executive leadership team began asking for completion of new risk assessments as they became available from the Child Health PSO. Depending on the type of risk assessment, the process will look different as stakeholders vary. But by using the existing infrastructure to complete risk assessments, the hospital has made progress to improve patient outcomes.