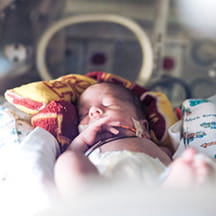
For parents of infants with serious medical conditions, a neonatal intensive care unit (NICU) represents more than just high-level medical attention—it's also an incredibly stressful and exhausting setting where they must make important decisions regarding their babies' care. Researchers at Johns Hopkins Children's Center suggest an often-overlooked component of NICU care—communication—is integral to successfully engaging parents in the critical dialogues that will ultimately affect long-term patient outcomes."Parents tell us what helps them engage in those conversations is if they feel like they can trust in, and are supported by, the neonatal intensive care unit staff," says Renee Boss, M.D., pediatric neonatologist and neonatal palliative care expert at Johns Hopkins Children's Center in Baltimore, Maryland. "Data suggests the quality of conversations parents have with the NICU staff is actually important to long-term outcomes. Parents who feel the quality of communication with the team was better are ultimately more satisfied with their babies' NICU care months and even years later."
Some conversations are more challenging
Boss says clear, understandable conversations are important to building that trust among all NICU families. But the research shows some conversations are more difficult to successfully navigate:
- Sudden diagnosis. When a child's diagnosis is sudden or unexpected, Boss says the family hasn't had time to prepare emotionally, which makes it harder for them to process the information.
- Long-term prognosis. According to Boss, the natural optimism of clinicians can sometimes confuse families facing difficult long-term prospects for their children. "Our data suggests those conversations don't always go particularly well," Boss says. "Families and clinicians often walk away with different ideas about what was said."
- Uncurable condition. "When it becomes clear there's no cure for what a baby has and is going to end up with chronic lifelong problems—and maybe even a shortened life span—that's hard news to share as well," says Boss.
Communication training not a priority
Despite the natural difficulties that conversations like these present to clinicians, Boss says most neonatologists don't receive formal communication training. In 2009, Johns Hopkins surveyed all graduating neonatology fellows across the U.S. to gauge what kind—and how much, if any—of communication training they'd received. Fellows representing 80% of the nation's programs responded, with fewer than half reporting any focused communication training. Most of the training that did take place seemed to only scratch the surface.
"The most common type of training was simply that they tagged along in a room with a senior clinician and watched them have a conversation," Boss says. "Very few fellows had had any sort of rigorous communication skills training."
Communication among care teams also essential
Boss says there's "robust data across multiple disciplines in medicine" supporting the benefits of targeted communication skills training to improve confidence and skills of clinicians.
As a result, Johns Hopkins has developed a communication skills course for neonate fellows. The course targets tangible communication skills that doctors can employ in a variety of clinical situations with patient families.
And because most NICU patients require a diverse multidisciplinary care team that can include dozens of clinicians across the hospital, there's a heightened potential for communication gaps among the care team. To address those potential communication gaps, Boss and her colleagues have also added training that focuses on team communications.
"We have to do a really good job communicating with each other, so we can work together to give those babies the best care possible," Boss says. "Our job is to all be on the same page, so we can walk forward together."